Osteoporosis
What is osteoporosis?
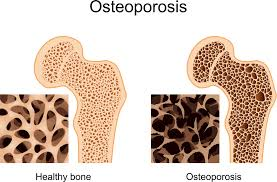
Osteoporosis is a condition where a person’s bones become thinner, more porous, decrease in mass, and are therefore at a greater risk of breaking.
What causes osteoporosis?
It is likely that a combination of factors cause this condition. Some of these factors include: diet, lack of exercise, menopause, weight (low) and use of steroid medication.
There are two main types of cells that help maintain bones: osteoblasts, which build up new bone; and osteoclasts which remove old bone. With age, osteoblasts become less efficient, so bone is taken away faster than it can be rebuilt. Additionally, as we age our digestive systems are less efficient at absorbing calcium from the food we eat. This means there are less resources available to rebuild bones. We reach a peak bone mass by our early twenties, and in our thirties it slowly starts to decrease and continues to decrease for the rest of our lives.
How is osteoporosis diagnosed?
Often there are no symptoms of osteoporosis until a fracture occurs. At this point, it is usually fairly advanced and cannot be fully reversed. This is why it is so important to take preventative measures early in life. Keep reading to learn how!
A detailed medical history can be used to assess your risk of fractures and osteoporosis. The gold standard in diagnosing osteoporosis is a bone mineral density scan (also known as DXA scan).
Who is affected?
In Canada 1 in 4 women over 50, and 1 in 8 men over 50 have osteoporosis. However, it can affect any age group. Even adolescents may develop osteoporosis if they are too active, such as elite athletes, if they suffer from anorexia, chronic inflammatory conditions, malabsorption syndromes, or take medication that increases bone loss. High alcohol intake, smoking, low body weight, low physical activity, steroid use (greater than 3 months) and poor diet are other factors that can contribute to osteoporosis at any age. Women over 50 are at the greatest risk due to menopause. Estrogen is protective to bones as it allows an increase in bone density. During menopause, estrogen levels decrease dramatically, which puts bones at risk for fracture.
How can it be prevented?
Building strong bones early on in life is the best way to avoid osteoporosis. This can be done by obtaining adequate calcium intake and doing weight-bearing activities by the time peak bone mass is reached (approximately 20 years old in men, and 16 in women).
Living an active lifestyle through all stages of life is helpful in preventing osteoporosis as well. It is important to get at least 30 minutes of moderate to intense physical activity each day, and to incorporate weight bearing and resistance exercise to ensure strong and healthy bones.
Resistance exercises causes osteoblasts to build bone and make them denser and stronger. You can add resistance to exercises with your own body weight, with resistance bands, or with weights and cable machines. Some exercises you can do with your body weight are: push-ups, squats, and lunges. Others that require equipment include: bicep curls, chest press, and rows. You should speak with your physician before starting a new exercise program.
Other exercises that are great for maintaining strong bones are weight bearing aerobic exercises, such as walking, jogging, stair climbing, and using an elliptical.
Speak with your Physiotherapist or Athletic Therapist if you have questions about exercising to prevent osteoporosis.
How can it be treated?
Once osteoporosis is diagnosed, it can be treated with medication and lifestyle changes. You and your doctor can decide which medication is best based on side effects, your specific needs and medical history.
Improving and maintaining balance is essential for preventing falls in all populations, but especially for those with osteoporosis. A great one to get started is standing on one foot (and holding on, if you need to). Some other functional exercises for working on balance are: walking on your heels only or toes only, walking heel-to-toe on a straight line forwards and backwards, and stand on one foot on an uneven surface (for example, a pillow).
Posture can be greatly affected by osteoporosis in the vertebrae. There are exercises that can help reduce the excessive curvature of the upper back that can occurs with vertebral fractures. These include strengthening the muscles of the upper with simply correcting your posture when you notice your slouching.
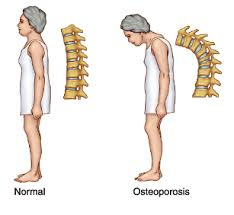
Yoga and tai chi are great for balance and can help with posture. However, positions and postures that involve bending forward are not suitable for individuals with osteoporosis (eg. trying to touch your toes).
If you have osteoporosis and would like to start exercising, speak with your doctor and a Physiotherapist to find an exercise program that works for you.

